
Exploring Effective Options for Chronic Migraine Relief; A Roadmap to Respite
I see patients stuck in the dark lonely rut of chronic migraine all day every day. Chronic migraine is a miserable headache disorder which causes

I see patients stuck in the dark lonely rut of chronic migraine all day every day. Chronic migraine is a miserable headache disorder which causes

Imagine a pain so intense that it feels like a storm raging inside your head, accompanied by a symphony of other symptoms that make even

If you experience headaches every day, you likely have a condition known as chronic daily headache. Generally speaking, the difference between episodic and chronic headaches
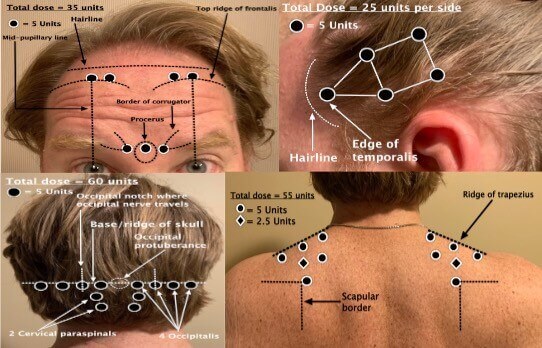
Botox for Migraines Botox for migraine headaches? This is often the response along with a confused look on a patient’s face when I discuss and
I see the worst of the worst headache, migraine, chronic migraine, facial pain, fibromyalgia, and chronic pain from many states and countries. I see patients

What is Rebound Headache (Medication Overuse Headache)? Rebound headache is also known as medication overuse headache (MOH). It is one of the most common causes
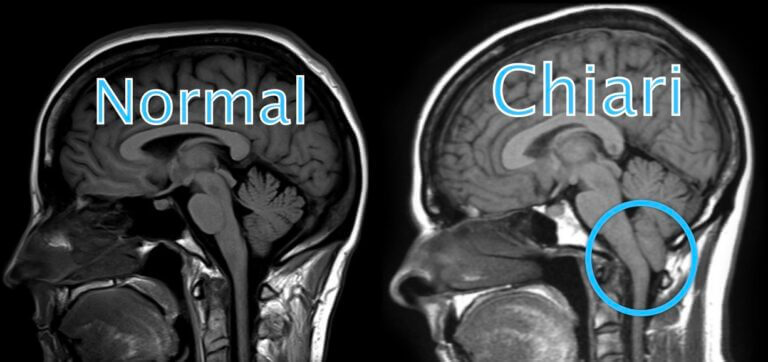
What Is Chiari Malformation? Chiari malformation, also known as Arnold-Chiari malformation, is a common congenital (born with it) condition of anatomical variation involving the brain